 Facing the possibility of colic surgery can be overwhelming for any horse owner. Knowing what to expect can help you make the best choice for your horse.
Facing the possibility of colic surgery can be overwhelming for any horse owner. Knowing what to expect can help you make the best choice for your horse.It’s 7 p.m. and your horse hasn’t touched his dinner. He’s sweating, pawing and looking at his side. He’s obviously in distress. Your vet arrives and, after an initial exam, confirms colic. But medical treatment doesn’t work and your horse remains in severe pain. Your vet starts talking surgery. What will you do?
Thankfully, althought colic itself is the second leading cause of equine death (after old age), only a small percentage of cases require surgery, according to David Freeman, MVB, PhD, Diplomate ACVS, Director of Island Whirl Equine Colic Research Laboratory at the University of Florida.
Still, when basic medical treatments fail to resolve the problem, you’ll need to make a decision quickly on whether to proceed with surgery. To make that choice under duress, you need to understand the ins and outs of colic surgery well before that time arrives. Here’s what you need to know.
Colic: Just the First Part Of a Diagnosis
“Colic is just the observation,” says Douglas Thal, DVM, Dipl. ABVP, Board Certified in Equine Practice, of Thal Equine LLC in Santa Fe, New Mexico. “It’s a demonstration of abdominal pain.” And it can be caused by a number of conditions, including gas, intestinal twists, loss of blood supply to the gut (ischemia), impaction and more.
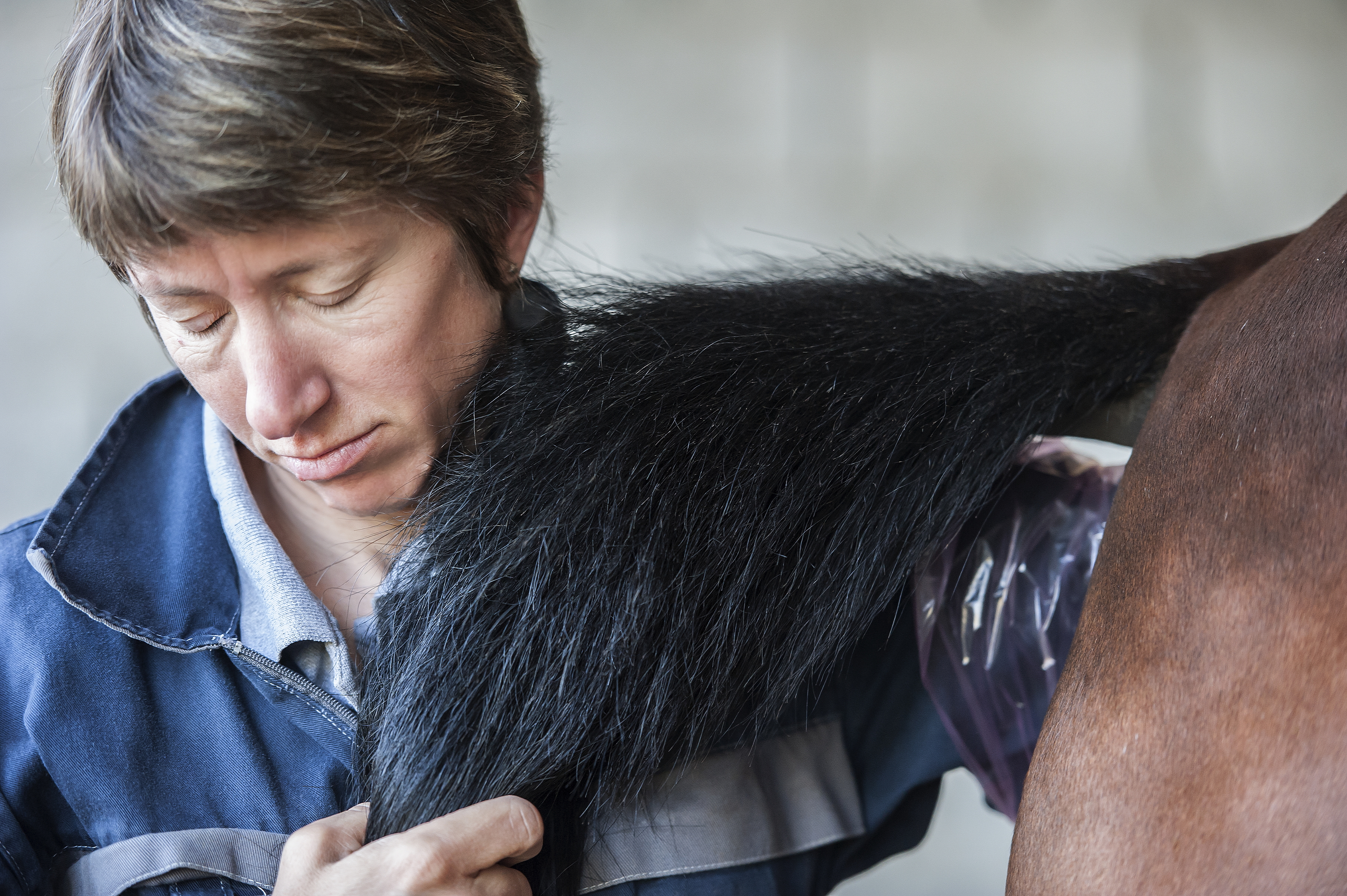 To help diagnose the cause of a horse’s colic, your vet will often perform a rectal exam to check for signs of a blockage or twist.
To help diagnose the cause of a horse’s colic, your vet will often perform a rectal exam to check for signs of a blockage or twist.To help determine which cause is at the root of your horse’s colic, your vet will likely conduct at least three basic tests in the field:
- A general physical exam, checking heart rate, temperature, mucous membranes and so forth
- A rectal exam to check for a blockage or twist
- Passing a nasogastric tube through the horse’s nostril to check for a blockage or twist (a nasogastric tube is passed through the horse’s nostril, through the pharynx, down the esophagus and into the stomach).
Your vet’s findings may add up to a diagnosis or at least suggest a treatment direction, says Dr. Thal. Or they may not. “You can have a horse whose vital signs are good, the belly fluid is normal, the rectal exam is normal, yet the horse is still in violent pain,” he says.
A reason for this potential lack of clarity is that the rectal exam and the nasogastric tube don’t “meet in the middle.” And in the gap is a region of the horse’s abdomen that can’t be easily examined, explains Shannon J. Murray, DVM, MS, Dipl. ACVS, of Littleton Equine Medical in Littleton, Colorado.
That’s why all three vets emphasize that colic surgery itself is the ultimate diagnostic test. In certain cases, it’s not until the horse is on the table and the vet is looking inside that a definitive determination of cause can be reached.
You Can’t Procrastinate
In many cases, even without a solid diagnosis, your vet will begin medical treatments to address your horse’s pain. Your horse’s reaction will provide more insights into whether this could be a surgical case.
“There’s a certain pattern we expect from a horse you’re treating in the field for nonspecific colic,” explains Dr. Thal. “A horse may respond to [an oral] dose of [the nonsteroidal anti-inflammatory drug] Banamine in 20 to 30 minutes. If the vet gives it [intravenously], then you can expect a response in five to 10 minutes. If you don’t get the response, you can chalk one up for this being a more serious condition.”
Your vet will also consider inherent risk factors that contribute to the decision. For instance, says Dr. Freeman, the following types of horses may need to be referred for surgery more rapidly than others:
- Horses over the age of 10 since they’re prone to developing fatty tumors, or lipomas, which can grow long “stalks” that may wrap around a horse’s intestine, strangulating the blood flow.
- Mares who foaled recently since they are prone to large colon volvulus, or twists–one of the most deadly forms of colic.
- Horses who have had recurrent bouts of colic since they could be more likely to have a condition that requires surgery.
- American miniature horses and ponies because they are prone to getting small colon impactions, which can require surgery.
When doubt remains, Dr. Freeman encourages owners to err on the side of caution and send their horse to the hospital sooner rather than later. “Not every horse referred will need surgery,” he says.
Furthermore, Dr. Freeman says, if your horse needs surgery, there is a better chance of requiring a simple procedure and having a better prognosis if you act quickly. He notes a German study of horses who had small-intestinal surgery. “Survival was 75.6 percent if surgery was performed within eight hours from onset of colic, compared with 45.1 percent survival in horses who had surgery 12 hours or more after onset of colic,” Dr. Freeman says.
 A horse suffering from colic will show signs such as pawing, sweating and looking at his sides.
A horse suffering from colic will show signs such as pawing, sweating and looking at his sides.Is Transport Risky?
While time is of the essence, you still need to consider some key factors before sending your horse to the hospital. First up: Can your horse be safely transported?
In straightforward colic cases, such as a gas distension or a minor intestinal displacement, the horse may arrive at the hospital much improved. There is some thought that the motion of trailering may actually help the horse, although the improvement could simply be due to the time lapse.
Length of trip can make a difference, and a shorter trip is better. But that doesn’t necessarily mean you shouldn’t risk a longer trip. Dr. Thal explains that his practice is one of only three in New Mexico and southern Colorado equipped for colic surgery. “I get horses from 3½ to 4 hours away. Most of the time, the horse can make the trip.”
Dr. Freeman agrees: “I have seen horses come long distances and arrive in bad shape but make it and benefit from the surgery.”
In some rare cases, says Dr. Thal, your vet may believe that your horse is not likely to survive the trip. But it’s hard to predict. It may be likely that the veterinarian will sedate your horse for transport to prevent him from thrashing and potentially traumatizing himself. Your vet may also ask you to stop during a lengthy trip to check your horse and possibly administer an intramuscular sedative injection if needed, he says.
Candidates for Colic Surgery
If you and your vet decide that your horse should be trailered, then your next consideration is the horse himself. While many owners believe older horses have poorer survival odds, some research studies have shown that’s not the case and these vets agree.
“Many of us have performed colic surgery on horses in their late 20s and 30s,” says Dr. Murray. “They may take longer to recover, but their prognosis can be similar to that of a younger horse.” (In fact, the day before we spoke, Dr. Freeman had completed a successful colic surgery on a 35-year-old horse who was recuperating nicely.)
More important is your horse’s overall health beyond the colic episode. The healthier he is in general, the better his chances of pulling through surgery and recovering well. If your horse isn’t in glowing health, your vet can help you understand how those ailments might affect his prognosis, says Dr. Thal.
Temperament also matters. Rehab typically means at least a month of stall rest with hand-walking. If your horse goes stir crazy in confinement, he may require long-term tranquilizers during rehab.
It’s Expensive (for a Reason)
One of the most important factors owners must consider is the cost of colic surgery. The procedure involves a large team of skilled veterinary staff, extensive equipment and intensive in-hospital post-surgical care. Specific costs vary by region, practice and type of surgery, with a range of approximately $5,000 to $12,000.
“The lower end of the estimate would likely be a simple large-colon displacement while the higher end of the estimate can often be reached with a large-colon volvulus [twist] or small-intestinal lesion,” says Dr. Murray. “And that’s without complications.” On top of that, you can expect another $600 or so for the initial/admit exam, she adds. (More details on that in a minute.)
“Colic surgery is not affordable for every owner,” says Dr. Murray. “And that is very fair and reasonable if they decide it’s not. Letting us know this information will help guide our treatment for the horse.”
If you have equine insurance that includes a surgical or major-medical policy, then cost may be less of an issue. You may still need to cover expenses up front and get reimbursed from the insurer later. And you’ll want to contact your insurance agent before the vet moves forward with surgery to make sure you’re following all the policy requirements.
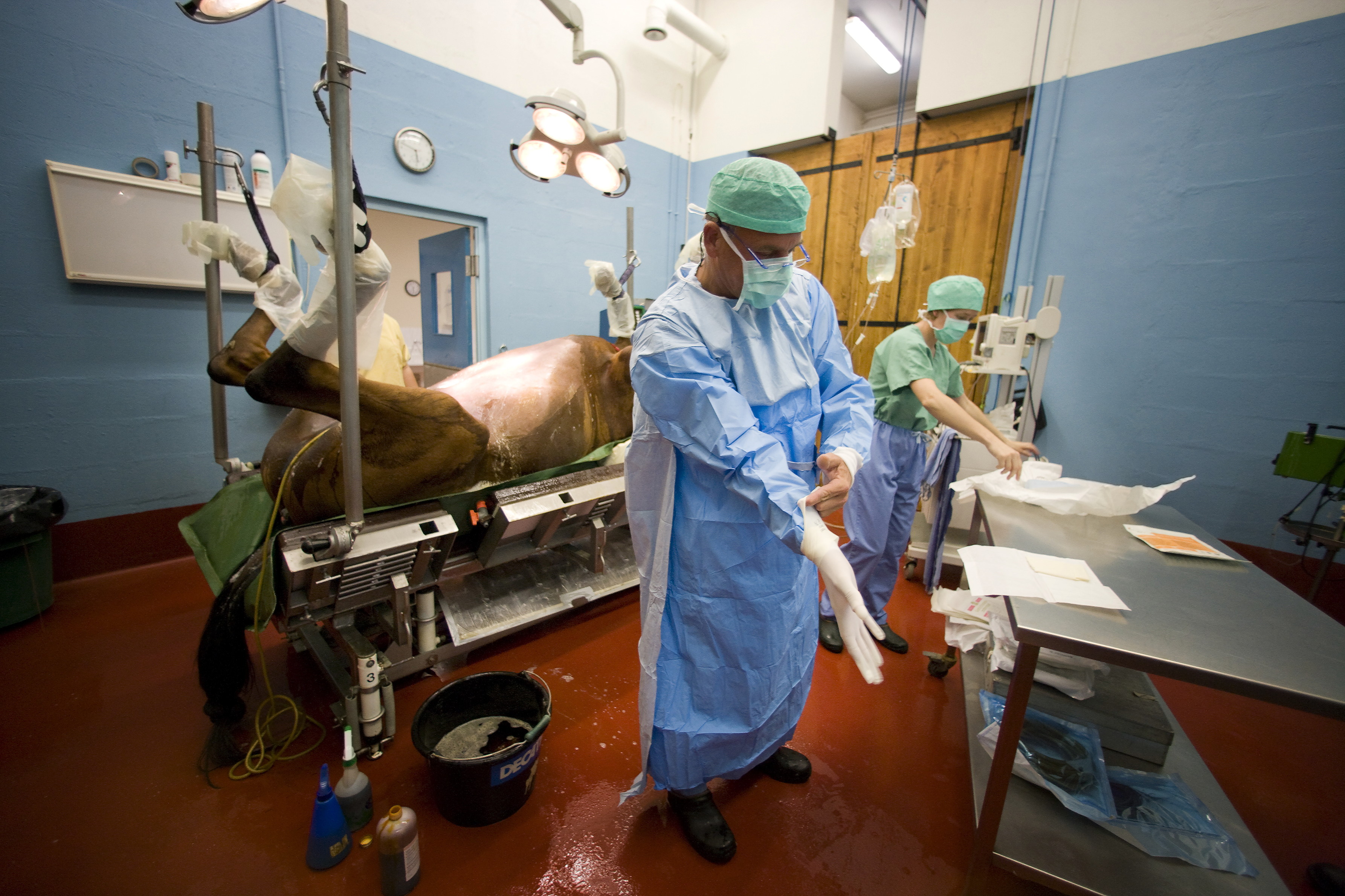
 If colic surgery is the plan, the horse will be anesthetized in a padded room and then transported to the surgery room, where the staff will prep him for the procedure.
If colic surgery is the plan, the horse will be anesthetized in a padded room and then transported to the surgery room, where the staff will prep him for the procedure.Arrival at the Equine Hospital
When your horse gets to the equine hospital, don’t be surprised when the staff doesn’t immediately lead him off to surgery.
“When your horse arrives at the clinic, he is examined again—including physical exam, blood work, nasogastric intubation, rectal exam, etc.,” says Dr. Murray. “Many of these diagnostics will have been performed by your veterinarian in the field, but things can change quickly when a horse colics, so the diagnostics may be repeated. This information helps determine the best course of treatment for your horse.”
It can also show whether your horse’s condition has improved or deteriorated, says Dr. Freeman.
Blood work is often run with results ready during the initial exam of your horse. Additionally, a sample of peritoneal fluid from the abdomen may be taken to gather more information. And the veterinarian may want to do an ultrasound as an additional diagnostic to literally try to get a better picture of what is going on in your horse’s abdomen, explains Dr. Murray. After the exam, she notes, the staff may place an IV catheter to administer fluids and drugs.
At this point, the vet may find that your horse’s colic can be managed without surgery. For instance, says Dr. Thal, a period of IV fluids and monitoring might be the next step in some cases. As another example, says Dr. Murray, with an entrapment, where the large colon is basically trapped between the kidney and spleen, modern drugs can be administered to help shrink the spleen. If the horse is then lightly exercised, the action may be enough to dislodge the large colon and solve the problem.
On the other hand, twists, strangulated intestines and many impactions or blockages must be handled in surgery.
 Colic surgery can take anywhere from 90 minutes to four hours, depending on the complexity of the case. Afterward, patients return to the padded room where they can wake up from the anesthesia in a safe, controlled environment.
Colic surgery can take anywhere from 90 minutes to four hours, depending on the complexity of the case. Afterward, patients return to the padded room where they can wake up from the anesthesia in a safe, controlled environment.You May Not Be Allowed to Watch
If your horse proceeds to surgery, some clinics will let you watch from a separate viewing area. Others won’t. If you don’t watch, make sure to stay accessible in person or by phone so that your vet can update you as the surgery proceeds. If you do watch, be prepared for what you’ll see. It can be tough to watch this scenario play out on your beloved horse.
In a nutshell, your horse will be taken to a padded room and anesthetized. Hobbles will be attached to all four legs and he’ll be hoisted, belly up, and transported to the surgery room. The staff will place a facial catheter to monitor blood pressure and an endotracheal tube for the anesthetic, explains Dr. Murray.
Once your horse has been placed on the surgery table, the prep begins. Dr. Murray explains that the staff will clip your horse’s abdomen from the groin (inguinal) region up to his sternum while the surgeon and assistant surgeon scrub in. Surgical drapes are then placed over your horse and the abdominal incision is made.
“The surgeon will then palpate the entire abdomen prior to removing any portion of the intestinal tract,” says Dr. Murray. “Following this, different portions of the intestinal tract [for example, large colon, small intestine, etc.] are then removed from the abdomen, examined and replaced in correct anatomic position.”
All Surgeries Are Not The Same
By now, your vet will likely have pinpointed the specific cause of your horse’s colic. He or she can then provide a better prognosis and may need to discuss next steps with you. If the problem is inoperable—for instance, in a place where the vet simply can’t reach—the recommendation may be euthanasia, says Dr. Murray.
If your vet thinks the problem is treatable, the rest of the procedure depends on the exact issue. Some of the more common procedures include the following:
- Severe impactions, which often involve large amounts of food or sand lodged in the pelvic flexure, a horseshoe-shaped curve in the colon. In these cases, the vet will lift the colon onto a special tray, make an incision and empty it. Special hoses will be used to keep the operating area clean and to help soften the impaction and flush the intestines.
- Resection and anastomosis. When part of the intestine has lost blood supply, the surgeon will cut out the damaged section (resection) and then sew the remaining pieces together (anastomosis).
- Twists and displacements. In these cases, the surgeon works to put everything back in its proper place. In some cases where the horse is having a second surgery for the same problem, the surgeon may opt to sew the colon to the body wall (colopexy) to prevent future displacement, says Dr. Freeman.
Depending on complexity, colic surgery can take anywhere from under 90 minutes to more than four hours in rare cases, says Dr. Thal. Afterward, your horse is returned to the padded room to wake up. Dr. Murray notes that at her clinic they’ll remove the horse’s shoes, tape the hooves and apply standing wraps to protect his legs during the recovery period.
 After surgery, horses typically remain at the vet hospital for up to a week, barring any further complications. Even after the sutures or staples are removed, it can often take months for the abdominal incision to fully heal.
After surgery, horses typically remain at the vet hospital for up to a week, barring any further complications. Even after the sutures or staples are removed, it can often take months for the abdominal incision to fully heal.Complications Now and Later
Once surgery is complete, your horse isn’t entirely in the clear. “While many of the simpler conditions rebound quickly, some horses can be very ill for days after surgery and almost always require prolonged and expensive intensive care,” says Dr. Thal.
In fact, you can expect your horse to stay at the hospital for about five to seven days. Treatment often includes IV fluids, antibiotics, painkillers and a gastric protectant, such as GastroGard, says Dr. Murray. “Additional treatments may be required and often depend on the specific case and the lesion found at surgery,” she says.
“Complications during this period include return to colic pain, abdominal infection, laminitis, colic recurrence, incision problems and others,” says Dr. Thal. But if a horse recovers well, the medical care and medications will decrease day to day. The veterinary staff will also gradually reintroduce your horse to his regular feed as soon as possible—ideally within 18 to 36 hours after surgery.
 After your horse returns home from surgery, he’ll need a strict rehab period to ensure the best chance for recovery. After a full month of stall rest and hand-walking, he can transition to a small paddock.
After your horse returns home from surgery, he’ll need a strict rehab period to ensure the best chance for recovery. After a full month of stall rest and hand-walking, he can transition to a small paddock.Rehab Takes Time
If all goes well, your horse should be home within a week. About two weeks after surgery, your vet will remove the staples or sutures closing the incision. But, says Dr. Thal, “It takes months for the abdominal incision to heal with much strength. Until healing of the abdominal wall takes place, exercise at speed must be avoided to prevent breakdown of the incision from stress.”
Specifically, says Dr. Murray, the rehabilitation process typically involves “a month of stall rest and hand-walking, then a month of stall rest and turnout in a small paddock. The third month is stall rest and turnout in a large paddock. In the fourth month, you can ride on the flat, and usually by the fifth month the horse can start jumping. That is, if there have been no complications.”
In general, your horse can return to his normal feed by the time he’s home, unless your veterinarian has discussed dietary modifications with you. You may want to dial back on grain to moderate his energy levels until he’s fully recovered, though.
Your horse may lose a little weight after surgery and may experience swelling along the incision. Dr. Murray says these aren’t concerns if they aren’t accompanied by other caution signs. For instance, Dr. Thal recommends contacting your vet if you see any of the following:
- Loss of appetite, depression or any change of attitude or behavior
- Increases in swelling or any drainage at the incision site
- Colic signs
- Swelling of the jugular-vein area of the neck that could indicate clotting of the vein after the catheter was removed
- Signs of laminitis, such as stiffness or soreness when walking.
Prognosis Varies
More than 60 years ago, colic surgery was considered a practically hopeless scenario, says Dr. Freeman. But today, we’re seeing survival rates of 75 to 90 percent. And most survivors are able to return to their previous performance levels. All three vets have seen colic-surgery patients recover and go on to continue careers in eventing, dressage, show jumping, endurance, racing and trail, sometimes at the highest levels of their sport.
An individual horse’s specific prognosis will depend on the type of lesion found at surgery, says Dr. Murray. The further your horse gets from surgery without experiencing complications, the better his long-term prognosis. The first 10 days have the greatest risk, then the first 100 days postsurgery. Risk diminishes after that and drops notably after one year, says Dr. Freeman.
Complications at this stage can include infections, adhesions (essentially “spot welds” of scar tissue between segments of intestine and body wall, other organs and other intestines), ileus (when the intestines’ normal and essential motion ceases), hernia at the incision site and laminitis.
And, of course, there is always the risk of recurrence. Certain colic conditions, such as displacements and twists, have a higher recurrence rate than others, say Drs. Freeman and Thal. But, notes Dr. Thal, any horse who has required colic surgery once may be prone to needing it again.
“[The horse] got into this situation in the first place and there’s a possibility that he’s going to do it again,” he says. “It’s not necessarily due to the colic surgery and the trauma. This is a population of horses that needed surgery in the first place, so depending on the specific condition treated at surgery, they may be more likely to have intestinal trouble.”
Still, he adds, “We do have those wonderful situations where 15, 20 years go by and the horse never has a recurrence.”
Be Prepared
Hopefully you and your horse will never face the possibility of a colic surgery. But if you do, understanding early on what’s involved—the price, the process and the prognosis—will help you make that do-or-don’t decision even under this most-trying of situations. And if surgery is the choice, then the faster you can decide to move forward, the more the odds will be in your horse’s favor.
Make a Plan
Having answers to the following six questions well before a colic crisis arrives will help you make a fast decision when you need to.
Where will you go? Not every equine veterinarian has surgical facilities. Talk with your vet to see if he/she does or can refer you to one or more qualified area hospitals that are equipped to handle colic surgery.
How will your horse get there? If you don’t have your own trailer or ready access to one, know how you’ll transport your horse to the hospital. Prepare now by asking your vet or local equine hospitals for recommendations of emergency transport companies. Dr. Shannon Murray suggests finding at least two options and keeping those phone numbers handy.
How will you pay? If you have equine insurance, make sure you understand what’s covered and what you need to do to ensure coverage in case of an emergency. If you don’t have insurance, consider researching policy costs and coverage or setting aside savings to build an emergency equine healthcare fund.
Where will your horse recover? Does your barn have the ability to accommodate your horse’s recovery, which will require stall rest and eventually a small individual turnout pen? Dr. Thal notes that he’s seen clients create makeshift stalls from portable corral panels. Just make sure the pen is secure and will keep your horse dry. Some veterinary hospitals may offer long-term boarding; ask about that option now if it might be a need later.
Who will help? During at least the first month of rehab, your horse will require hand-walking multiple times every day. Some horses become hard to handle during stall confinement, looking for ways to release pent-up energy. Will you be able to personally handle the task? If not, do you have friends, family or barn crew who will help out?
What will your choice be? Have at least a tentative plan for what conditions might sway your choice to have or not have surgery. But give yourself the flexibility to revise your decision if the need arises.
This article was originally published in the July 2017 issue of Practical Horseman.