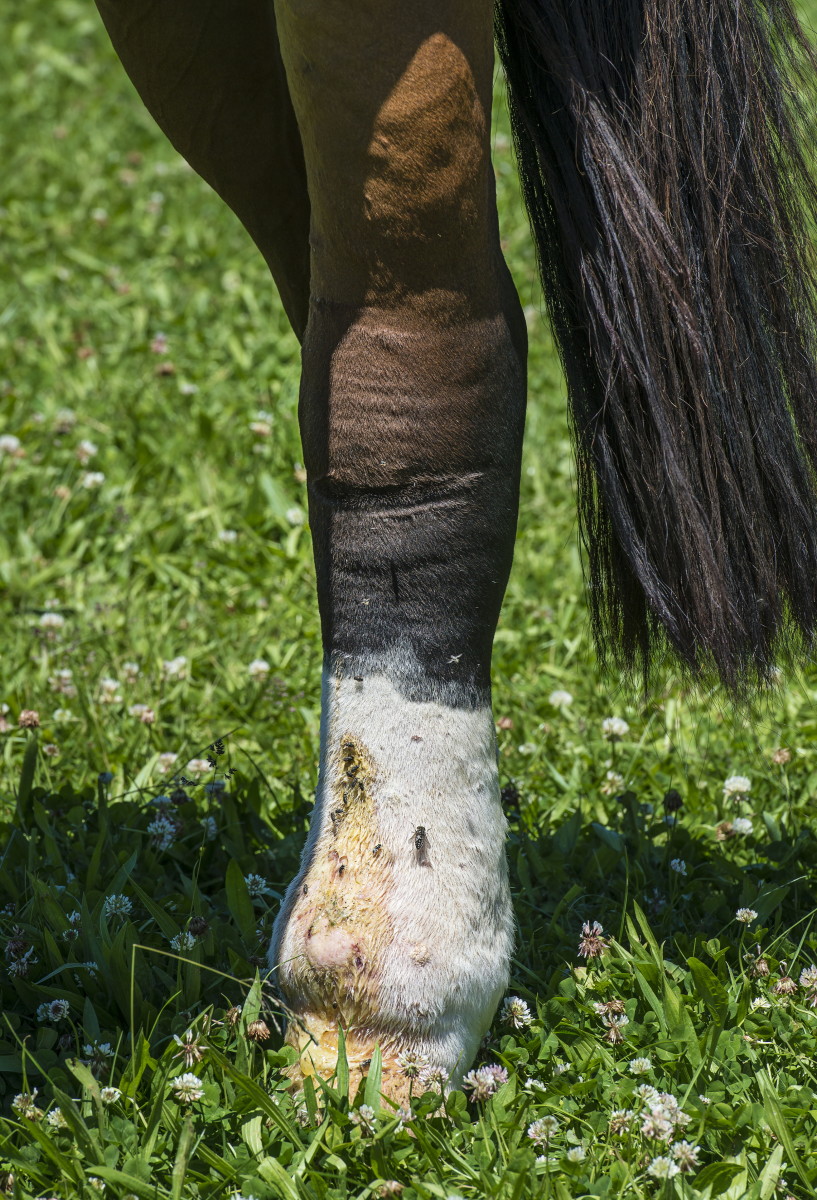
Your horse was fine when you left him in his stall last night, but this morning he’s moping in a corner, reluctant to step out. It doesn’t take you long to see the problem—from hoof to well above the hock, his left hind leg is swollen to twice its normal width. That extreme swelling can be a hallmark of cellulitis, a condition that can be life-threatening in horses.
“It should be treated the day you observe it, before the sun goes down,” says Emma Adam, BVetMed, PhD, DACVIM, DACVS, at the Gluck Equine Research Center, University of Kentucky. In this article, Dr. Adam helps explain what you need to know about cellulitis.
Cellulitis and its close cousin lymphangitis produce similar signs, and both are caused by microbial infections. In cellulitis, bacteria infect the tissues under the skin; in lymphangitis, bacteria infect the lymphatic ducts that drain fluid from the limb. The terms are often used interchangeably, and the signs and treatments are substantially the same. Either way, “The horse needs a veterinarian,” says Dr. Adam.

Sudden and Severe
Cellulitis comes on fast, typically blowing up in less than 12 hours. It stands out from other types of leg swelling in several ways.
- Extent. “The ‘stovepipe’ leg, with extensive swelling and loss of normal contours, is a classic sign,” Dr. Adam says. “Swelling related to injuries is typically more localized.” The full length of the limb, from foot to stifle, may be swollen.
- Distribution. The swelling classically occurs in one leg, most often a hind leg. It’s less common in front or in multiple limbs unless there are inciting reasons such as infected wounds. It’s not clear why hind limbs are affected more often than front. “Kicking may make hind legs more prone to injuries that trigger the condition [wounds, blunt-force trauma], or the hind legs may be more difficult to clean properly, so small injuries and skin conditions may be missed,” Dr. Adam says.
- Heat. A leg with cellulitis feels warm to the touch. The skin is taut and stretched and may even ooze fluid.
- Pain. Cellulitis is extremely painful, and the horse may not tolerate any pressure on the swollen limb. He may resist efforts to handle the leg and may be unwilling walk on it.
- Fever. An elevated temperature is common, especially in severe cases. The horse may seem depressed or go off his feed.
The bacteria identified in these infections are typically Staphylococcus and Streptococcus species, although other types can be involved. These bacteria are common in the environment and on the horse’s skin. Trouble starts when they get through a break in the skin—a cut or an abrasion, a surgical incision, a hock injection (rare), even severe chapping or a case of scratches. Sometimes no break in the skin is found, but the skin can be damaged by blunt trauma. “How it gets started in those cases isn’t clear. Perhaps blunt force trauma damages circulation or there is a break in the skin too small to observe,” Dr. Adam says.
Once the bacteria are in, they multiply and produce toxins that cause widespread inflammation and damage to blood and lymphatic vessels. Fluid leaks from the damaged blood vessels, and the impaired lymphatic system struggles to drain it away. Swelling builds, further restricting circulation.

Arnd Bronkhorst
Severe cellulitis can do permanent damage and leave the horse with a lasting lameness. Some of the biggest risks come from potentially fatal complications. Chief among them are:
- Laminitis. If the horse’s left hind leg is severely sore, he’ll keep his weight on the right hind, the contralateral limb. Weight-bearing laminitis can develop in the contralateral limb, and the risk grows as time goes on. Laminitis is defined as inflammation of the laminae in the hoof wall—the structures that hold the hoof to the pedal bone (coffin bone). The end result is pain and can also be a loss of strong attachment of the hoof wall to the coffin bone. This loss of structural integrity can lead to rotation of the coffin bone or in cases where the damage is circumferential, the sinking of the coffin bone leading to penetration of the sole of the hoof. Impaired circulation is also thought to be a trigger that can cause laminitis in the limb affected by cellulitis. Laminitis is an extremely painful condition that that may lead to euthanasia.
- Dermal necrosis. Bacterial toxins can have direct effects on the skin, causing significant damage. In addition, impaired circulation chokes off the supply of oxygen and other vital nutrients to skin cells. The skin dies and sloughs off, leaving tissues below exposed. Complications arising from skin sloughing include septic joints and tendon sheaths. Bacteria associated with cellulitis can produce toxins that lead to septic-shock syndrome, sepsis and multiple organ failure.
“You want to nip the infection in the bud,” Dr. Adam says. “If you leave it for a day or two, it can be much harder to control.”
What To Do
Call your veterinarian immediately if you suspect cellulitis. Treatment aims to limit damage and prevent complications by stopping the infection, reducing swelling and getting the horse comfortable as quickly as possible.
- Antimicrobial drugs. Your veterinarian will prescribe an appropriate antibiotic but may also take samples for culture, if possible. Imaging the limb with ultrasound may locate a site where a sample of fluid can be drawn for testing to identify the bacteria. “Historically, we have been reluctant to draw fluid for testing out of fear that puncturing the stretched skin will cause it to split. But there’s no evidence of this in the published reports, and the test results can help the vet choose the most effective antimicrobial drug,” says Dr. Adam.
- Anti-inflammatory drugs. Systemic nonsteroidal anti-inflammatory drugs such as flunixin meglumine or phenylbutazone serve two functions: reducing swelling and combatting discomfort. Your veterinarian may also prescribe a topical anti-inflammatory such as diclofenac cream or gel, which can be applied to skin in the affected area if appropriate. Dr. Adam suggests exercising caution if using these products, especially if the limb is to be bandaged because the skin is already stressed by swelling and poor circulation.
- Cold therapy. Cold helps reduce swelling and slows bacterial activity. Ice—an ice boot or ice packs—is most effective. The limb may be iced for 20 to 30 minutes every hour or on a schedule set by the veterinarian. “Change the ice frequently,” Dr. Adam cautions. “Once ice packs warm, they actually hold heat in the leg. The effect of cooling the limb cannot be overemphasized—it really helps.” If ice isn’t available, cold water from a hose can be used instead. Be sure to use a gentle stream, not a forceful blast. The skin is under stress—stretched by swelling and attacked by bacterial toxins—and can be easily damaged. For the same reason, gently pat the leg dry after hosing.


- Bandaging. Supportive wraps are sometimes used to limit swelling, but they can be tricky in cellulitis because they may hold in heat. After a bandage is applied, areas above the wrap often swell, which can cause problems in that area. In any case, the limb may be so painful in the initial stages that the horse won’t tolerate a pressure wrap. “I prefer to wrap the leg very lightly with a thin, compressive layer and then get it into the ice boot,” Dr. Adam says.
- Movement. Activity stimulates circulation in the leg, which will help speed recovery. Once the horse’s pain starts to subside and he’s comfortable walking, put him in a large stall or a medical paddock where he can move around at will without overdoing it. You can also hand-walk him for short sessions—say, five or 10 minutes—several times a day.
Monitor the condition closely. “The horse should get better with treatment,” Dr. Adam states. If swelling doesn’t start to decrease or the horse’s comfort level doesn’t improve after a day or two of treatment, it’s time to consider additional steps.
Stubborn Cases
Ultrasound scans can help your veterinarian monitor the course of the condition and identify pockets of infection. If initial treatment doesn’t bring results, a range of other therapies may.
- Switching drugs. This is often considered in difficult cases, and it’s an obvious step if the fluid drawn from your horse’s leg shows bacteria that are not responsive to the antimicrobial he’s getting. But in cellulitis, even the right drugs may not knock out the bacteria, Dr. Adam says: “Antibiotics can only work if they’re delivered to the site of infection. The swelling and disruption in blood flow caused by cellulitis can make this difficult.” Switching antibiotics is not a risk-free choice, and the use of multiple antibiotic drugs can increase the risk for antibiotic-associated diarrhea.
- Better methods of drug delivery. IV regional limb perfusion is one way to get more medication to the site. With the horse sedated, the veterinarian applies a tourniquet above the affected area and then injects suitable diluted antimicrobial into a vein below the tourniquet. After about 30 minutes the tourniquet is removed. This procedure is repeated on a schedule determined by the veterinarian, but only if the limb can tolerate it.
- Surgical drainage. In some cases pockets of infection linger even with appropriate therapy. “Drainage allows better circulation in these stubborn sites,” Dr. Adam says. “A recent case study indicated that surgically draining pockets of infection, using advanced ultrasound imaging as a guide, can help bring about resolution of problematic cases.” Depending on the case, the procedure is done at a clinic or equine hospital under general anesthesia or standing with the horse sedated.
- Next-level pain relief. “The longer the horse goes without using the affected limb, the greater the risk of weight-bearing laminitis in the contralateral limb,” Dr. Adam notes. If NSAIDs don’t do the trick, the veterinarian can turn to a range of pain meds, including opioids, administered locally or systemically. For hind-limb cellulitis such medications can be delivered by epidural injection just above the tailhead. Systemically, fentanyl transdermal patches may be applied to an area of normal skin and changed every 48 to 72 hours for adequate pain control.
Several adjunct therapies can be used to help horses recover from cellulitis. One option is hyperbaric oxygen therapy, available at some clinics and rehab centers. The horse spends an hour or so each day in a special chamber, breathing pure oxygen at two or three times atmospheric pressure. Evidence indicates that the treatment increases the delivery of oxygen to tissues, reduces swelling and enhances the effects of some antibiotics.
Paula da Silva/arnd.nl
Looking Ahead
Horses treated promptly usually make a full recovery from cellulitis, often within days. The outlook is more guarded when the infection is extensive or when treatment is delayed or doesn’t bring some improvement within 24 to 48 hours. The risk of damage to tissues and circulation increases in those cases, and some damage may be permanent.
Even when the horse makes a good recovery and returns to work, “The affected leg may not completely regain its normal contour,” Dr. Adam says. The lingering swelling is a sign that there’s some degree of permanent damage.
Horses who have had one bout of cellulitis may also be prone to recurrent episodes. Because activity promotes circulation in the legs, these horses can benefit from as much turnout time as possible. Standing wraps may help keep puffiness at bay when they’re stalled.
Good horsekeeping is the best way to guard against an initial or repeat attack of cellulitis. “Hygiene is linked to cellulitis in human medicine,” Dr. Adam says. “While the connection hasn’t been demonstrated in horses, it makes sense that hygiene could be a factor.” Mud, muck and dampness irritate skin and make it an easy mark for infections. So:
- Be fussy about the care of your horse’s skin and coat with special attention to legs and feet. Keep legs clean, and dry gently but thoroughly after bathing.
- Check regularly and carefully for skin irritations and cuts. Even tiny nicks and cuts should be cleaned and treated appropriately.
The key point to remember about cellulitis, Dr. Adam says, is to jump on it at the first sign. “Calling your veterinarian is excellent value for money compared to the extensive problems you’ll face if it gets away from you.”
Sidebar: Cellulitis or …
Cellulitis may be the most dramatic cause of limb swelling in horses’ legs, but it’s far from the only one. Here are three of the most common.
Stocking up is a buildup of fluid (edema) in the lower leg, typically in both hind legs but sometimes in all four. The horse isn’t lame, and the swelling is cool and not painful to the touch. If you press it with a fingertip, a slight depression remains for a moment after you remove your finger. Many horses stock up when they’re stalled because inactivity slows circulation, allowing fluid to accumulate. Activity generally brings the swelling down.
Windpuffs are soft, fluctuant swellings that appear just above the ankles, around the flexor tendons (the major tendons at the back of the legs). They’re caused by fluid that collects in the synovial sheaths, the casings that enclose the tendons, and the fetlock joint, and are typically thought to be the result of wear and tear of the tendon and joint. As long as windpuffs are cool, soft and not painful to the touch, they’re no cause for concern. Heat, soreness or lameness could signal more serious problems, though.
Injuries produce swelling along with other signs. Blood and lymph fluid leak into injured tissues, and body chemicals trigger inflammation that produces heat and soreness. Swelling tends to be localized at the injury site.
Leg injuries range from minor scrapes to torn tendons and fractured bones. The horse needs prompt veterinary attention if he’s markedly lame or in pain or if he has a puncture or a cut that needs stitches or may involve a joint or tendon. Any cut, even a minor scratch that’s treated with first aid, should be kept clean and dry and monitored carefully for signs of infection—discharge or heat, pain and swelling that persist beyond a day or two.
This article originally appeared in the Summer 2020 issue.